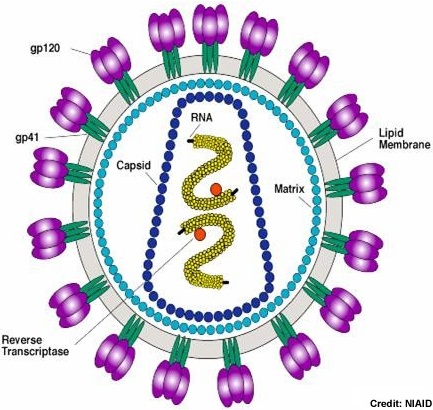
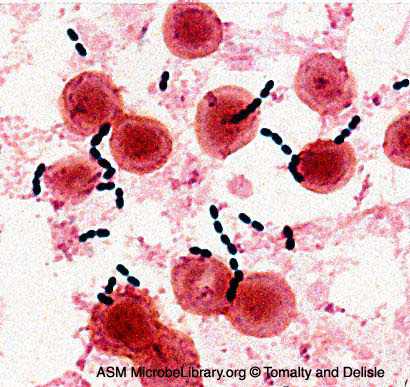
This patient presented with stroke. This article reviews stroke in IE. This related article reviews the neurologic manifestations of IE.
This patient presented with stroke. This article reviews stroke in IE. This related article reviews the neurologic manifestations of IE.An original article by Osler on IE!
Some key points:
Mitral Valve IE ~ 10% stroke rate
Mortality is high -- 35% in hospital 52% at one year
Early antibiotic therapy reduces neurologic complications
I have previously blogged about infective endocarditis (see here) including enterococcal endocarditis. The first post goes over the Duke Criteria.
Indications for Surgical Treatment of IE (Native Valve):
- Development of heart failure
- MR/AR with dilating LV, or development of pulmonary hypertension
- Fungal IE or that caused by highly resistant organisms (think of it in MRSA)
- Patients with heart block, cardiac abscess, abnormal chamber-chamber connections
- Recurrant emboli despite ABX
- Class IIb -- large vegetations